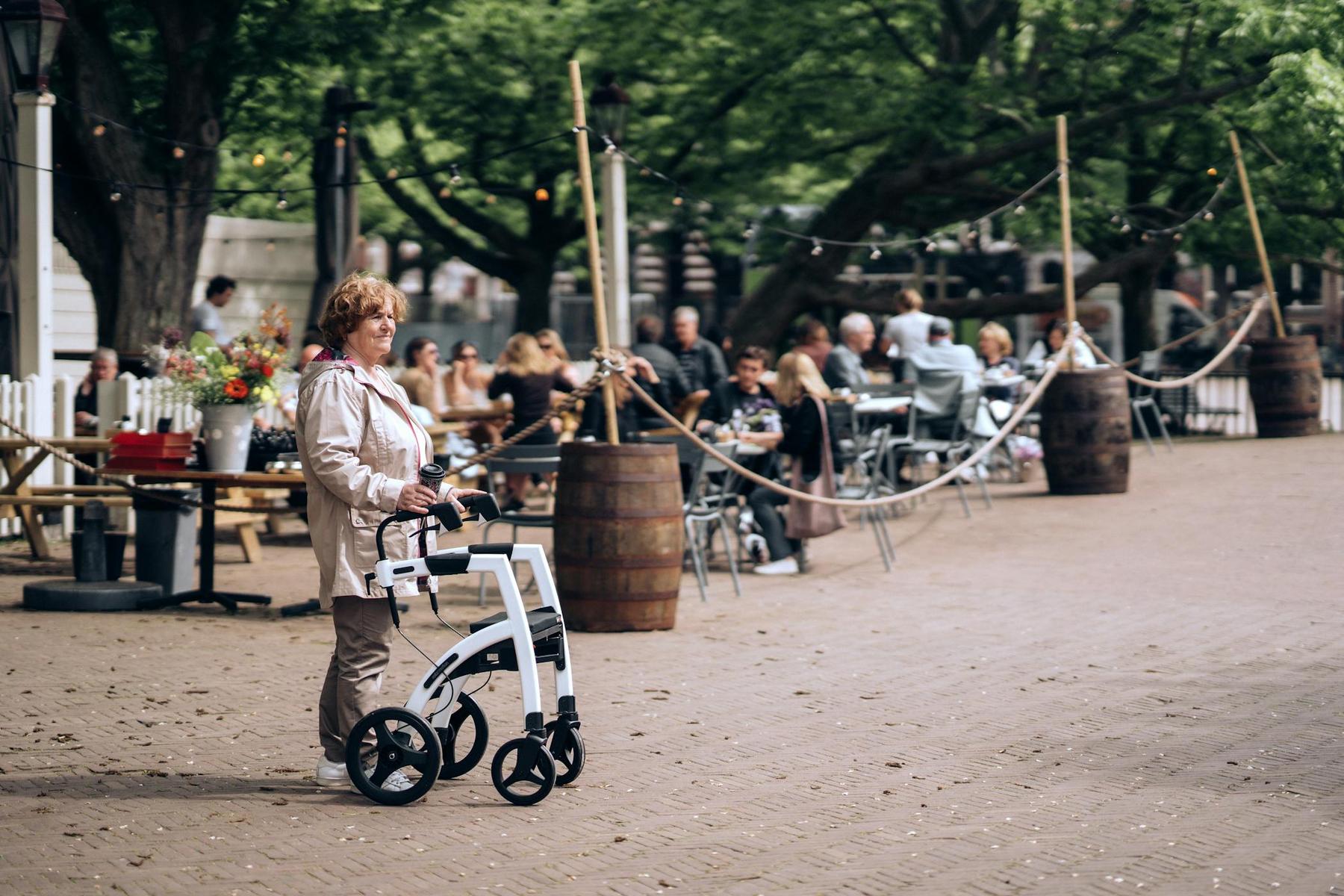Walking should feel empowering – not exhausting. Yet for many Australians living with chronic illness, disability, neurological conditions, or the effects of ageing, the simple act of moving from one room to another can demand far more energy than most people realise. When you or someone you care about relies on a walking aid – whether a cane, crutch, walker, or rollator – the physical and cognitive demands of locomotion change significantly.
Understanding energy conservation while walking with aids is not simply a clinical strategy. It is a meaningful pathway to greater independence, reduced fatigue, and a better quality of life. For NDIS participants, aged care recipients, and private clients across Brisbane, North Lakes, the Gold Coast, Sunshine Coast, Sydney, Melbourne, and beyond, learning how to work smarter – not harder – when mobilising with an aid can genuinely transform daily living.
Why Does Walking with Aids Use More Energy Than You Might Expect?
The human body is remarkably engineered for efficient movement. Under normal circumstances, walking at intermediate speeds of approximately 1.4–2.0 metres per second is metabolically optimal. The stance phase of walking is approximately three times more energy-intensive than the swing phase, with hip extensors consuming roughly 40% of total muscle energy expenditure, ankle plantar flexors approximately 27%, and knee extensors around 18%.
When a walking aid is introduced into this equation, the biomechanical picture shifts considerably. In healthy, younger users who are new to cane use, research has found an increase in energy expenditure – largely attributed to the heightened cognitive demands of learning a new motor pattern. Conversely, individuals who genuinely rely on a walking aid for stability and weight-bearing tend to demonstrate decreased energy requirements with correct aid use, because the aid reduces load on compromised limbs and improves gait stability.
This distinction is central to energy conservation while walking with aids: it is not simply about slowing down – it is about optimising how the entire body and mind work together during movement.
In older adults, the physiological cost of walking rises further due to factors such as reduced hip extension, altered walking cadence, diminished aerobic capacity, and less coordinated muscle activation. These changes make understanding energy conservation while walking with aids especially relevant for aged care recipients and those managing age-related mobility changes.
Which Walking Aid Is Most Energy-Efficient?
Not all walking aids are equal in their impact on energy expenditure. The design and type of aid significantly influences how much energy a person uses during mobility – a key consideration when selecting appropriate equipment.
| Walking Aid | Relative Energy Efficiency | Key Benefit | Potential Consideration |
|---|---|---|---|
| Standard (non-wheeled) walker | Lower efficiency | High stability and support | Requires lifting – increases upper limb demand |
| Rollator (wheeled walker) | Higher efficiency | Minimises energy cost compared to non-wheeled walkers | Requires attentional awareness on inclines |
| Single-point cane | Moderate | Lightweight and easy to use | Limited support for significant balance deficits |
| Quad cane | Moderate-high | Greater base of support | Slightly heavier; may slow walking speed |
| Crutches (swing-through gait) | Energy-intensive but fast | Greater speed is possible | High upper limb and cardiopulmonary demand |
| Mobility scooter / wheelchair | Minimal walking energy required | Maximum energy conservation for mobility | Reduces opportunity for active ambulation |
Rollators consistently demonstrate reduced energy expenditure and improved gait efficiency compared to standard non-wheeled walkers. This is important practical information for occupational therapy assessments, where selecting the right aid is central to supporting energy conservation while walking with aids.
Environmental design also plays a meaningful role. Research shows that handrail use during treadmill walking produced a 16% decrease in energy consumption in chronic stroke patients, and external stabilising frames reduced energy cost by 6% in non-pathological gait and 10% in pathological gait conditions such as spinal cord injury.
Who Benefits Most from Energy Conservation While Walking with Aids?
Energy conservation strategies and walking aid use are relevant across a broad range of conditions and populations. While every individual’s experience is unique, there are common presentations where an occupational therapist may explore these approaches as part of a wider support plan.
Chronic and Neurological Conditions
Conditions that place elevated demands on the cardiopulmonary or neuromuscular systems include:
- Chronic Obstructive Pulmonary Disease (COPD)
- Multiple Sclerosis (MS)
- Parkinson’s disease
- Post-stroke recovery
- Amyotrophic Lateral Sclerosis (ALS)
- Congestive heart failure
- Rheumatoid arthritis
- Spinal cord injury
- Cerebral palsy
- Osteoarthritis
Aged Care and NDIS Populations
For aged care recipients experiencing declining aerobic capacity, and for NDIS participants with mobility-related disabilities, energy conservation while walking with aids forms a core component of daily living support. Occupational therapists assess participants’ goals, home environments, and functional capacity to provide tailored strategies and assistive technology recommendations suited to each person’s circumstances.
Post-Surgical Recovery
Individuals recovering from joint replacement or other orthopaedic procedures frequently use walking aids during rehabilitation. During this period, understanding energy conservation principles supports recovery and helps prevent unnecessary fatigue.
How Can the Six P’s Framework Guide Energy Conservation While Walking with Aids?
Occupational therapy practice draws on a widely recognised framework of six core strategies – commonly referred to as the Six P’s – to guide energy conservation during daily activities, including mobility with an aid.
1. Prioritise
Identify which activities matter most each day. Reserving energy for meaningful mobility tasks – such as walking to the letterbox, attending a medical appointment, or visiting a community space – may mean thoughtfully rescheduling lower-priority activities.
2. Plan
Before beginning any mobility task, plan ahead. Gather everything needed before moving so that unnecessary walking trips are avoided. Organise your environment so frequently used items are within easy reach. Planning regular rest breaks into the daily schedule is equally important.
3. Pace
Maintain a slow, steady pace when walking with an aid. A useful general guide is approximately 10 minutes of rest per hour of activity. Rushing significantly increases energy expenditure and elevates fall risk. Pacing also means breaking longer distances into shorter segments with planned rest stops.
4. Position
Sitting requires approximately 25% less energy than standing for equivalent tasks. Whenever feasible, complete activities from a seated position. Maintaining upright posture – whether sitting or standing – reduces musculoskeletal strain. When resting between mobility tasks, positioning hips slightly higher than knees helps ease the transition back to standing.
5. Postpone
It is entirely reasonable to postpone non-essential activities on high-fatigue days. Asking family members, carers, or support workers for assistance is a sound energy management strategy. Delegating lower-priority tasks preserves energy reserves for activities that are most meaningful.
6. Problem-Solve
Consider how an activity might be modified to require less effort. Could a wheeled trolley replace carrying grocery bags? Could a shower chair eliminate the energy cost of prolonged standing? Adaptive equipment and environmental modifications are powerful problem-solving tools that directly support energy conservation while walking with aids.
What Adaptive Equipment Supports Energy Conservation While Walking with Aids?
Beyond the walking aid itself, a broad range of adaptive equipment supports energy conservation throughout the day. Occupational therapists assess which tools are most likely to benefit each individual based on their specific circumstances and goals.
Mobility and Transfer Aids
- Rollators with built-in seats for rest breaks during longer distances
- Lift chairs to reduce the energy required to transition from sitting to standing
- Grab bars and handrails to improve confidence and reduce reliance on lower limb effort
- Transfer benches for safe, seated bathing
Daily Living Equipment
- Long-handled reachers and grabbers to eliminate bending and excessive reaching
- Sock aids and long-handled shoehorns for seated dressing
- Wheeled trolleys for transporting items without carrying
- Electric appliances – such as electric can openers and blenders – to reduce manual effort in the kitchen
Bathroom and Personal Care
- Shower chairs or bath benches with back support
- Handheld shower heads for seated bathing
- Raised toilet seats to reduce effort during sit-to-stand transfers
The combination of appropriate adaptive equipment and energy conservation techniques can make a meaningful difference – not only in how tasks are completed, but in how individuals feel about their capacity to manage daily life independently.
NDIS Assistive Technology Funding in Australia
For eligible NDIS participants across Queensland, New South Wales, Victoria, and Tasmania, assistive technology – including walking aids and other adaptive equipment – can be funded through the NDIS. Funding is structured across four levels of complexity:
- Level 1 – Basic (under $1,500): Includes walking sticks and basic shower chairs; accessible through the Core budget with no formal assessment required
- Level 2 – Standard ($1,500–$15,000): Includes transfer benches and basic wheelchairs; requires a professional recommendation letter
- Level 3 – Specialised (varies): Includes power wheelchairs and mobility scooters; requires a formal assistive technology assessment
- Level 4 – Complex (over $15,000): Includes custom seating systems and ceiling hoists; requires a comprehensive assessment and detailed report
An occupational therapist can conduct the necessary assessment, trial appropriate equipment in a real-world environment, and prepare supporting documentation for NDIS submission.
How Does an Occupational Therapist Support Energy Conservation While Walking with Aids?
Occupational therapists are well-positioned to address energy conservation while walking with aids because of their training in activity analysis, biomechanics, ergonomics, and assistive technology. An assessment in this area typically involves the following components:
- An in-depth interview to understand your goals, challenges, and daily routines
- Observation of how you currently complete functional mobility and daily living tasks
- Assessment of your home or community environment for barriers and potential supports
- Evaluation of physical, cognitive, and sensory factors that may influence mobility
- Trialling different walking aids or adaptive equipment within your real environment
- A review of your current aids to assess whether they are correctly fitted and appropriate for your needs
Following assessment, the occupational therapist may recommend a combination of energy conservation education, environmental modifications, adaptive equipment trials, and – where appropriate – assistive technology funding applications through the NDIS or other funding pathways.
Research indicates that even a single targeted session of energy conservation training can produce meaningful reductions in fatigue, breathlessness, and perceived exertion during daily activities. More intensive programmes spanning several weeks demonstrate broader improvements, including increased walking distance and greater participation in community life.
For clients across Brisbane, North Lakes, the Gold Coast, and Sunshine Coast communities including Noosa, Buderim, Peregian Springs, and Gympie, as well as Sydney and Melbourne, Astrad Allied Health provides mobile occupational therapy services delivered directly in the home or community. Telehealth services are also available for clients across much of Queensland, New South Wales, Victoria, and Tasmania – ensuring that access to professional support is not limited by geography.
Making Every Step Count
Energy conservation while walking with aids is about far more than managing tiredness – it is about protecting your capacity to live fully, engage meaningfully with your community, and pursue the activities that matter most. Whether you are navigating a chronic health condition, recovering from surgery, living with a disability, or supporting a loved one through any of these experiences, evidence-based energy conservation strategies offer a practical foundation for more efficient, confident, and sustainable daily movement.
The right aid, correctly fitted and appropriately used alongside tailored energy conservation strategies, can meaningfully reduce physiological demands and support participation in the activities that make life worthwhile. An occupational therapist can work with you to bring all of these elements together in a way that is specific to your needs, your environment, and your goals.
Have questions? Need help? Contact Astrad Occupational Therapy today.
What is energy conservation while walking with aids, and why does it matter?
Energy conservation while walking with aids refers to the use of evidence-based techniques, strategies, and adaptive equipment to reduce the physical effort and fatigue associated with aided mobility. It is particularly relevant for individuals living with chronic conditions, disability, or age-related changes, as it enables greater participation in daily activities while protecting available energy reserves.
Does using a rollator or walker actually reduce energy expenditure?
Research indicates that for individuals who genuinely rely on walking aids for stability or weight-bearing support, correct aid use can reduce overall energy requirements compared to unsupported ambulation. Rollators – wheeled walkers – have specifically been shown to minimise energy cost compared to standard non-wheeled walkers, making them a meaningful option when energy conservation is a priority.
Can an NDIS participant access funding for walking aids and adaptive equipment in Queensland?
Yes. NDIS participants may be eligible for assistive technology funding – including walking aids and daily living equipment – through their NDIS plan. The level of funding and the required process depends on the complexity of the equipment. An occupational therapist can assess individual needs, recommend appropriate equipment, and prepare the supporting documentation required for NDIS submissions.
How do I access an occupational therapy assessment for energy conservation in Brisbane or via telehealth?
Astrad Allied Health provides mobile occupational therapy services across Brisbane, North Lakes, the Gold Coast, Sunshine Coast, Sydney, and Melbourne, with telehealth services available across Queensland, New South Wales, Victoria, and Tasmania. An occupational therapist will assess your needs within your home or community environment and provide individualised recommendations.
Which conditions benefit most from energy conservation techniques when walking with aids?
Energy conservation while walking with aids is relevant across a wide range of conditions, including COPD, multiple sclerosis, Parkinson’s disease, post-stroke recovery, rheumatoid arthritis, heart failure, spinal cord injury, and age-related mobility changes, among others. Occupational therapists provide individualised guidance based on each person’s specific circumstances, goals, and environment.